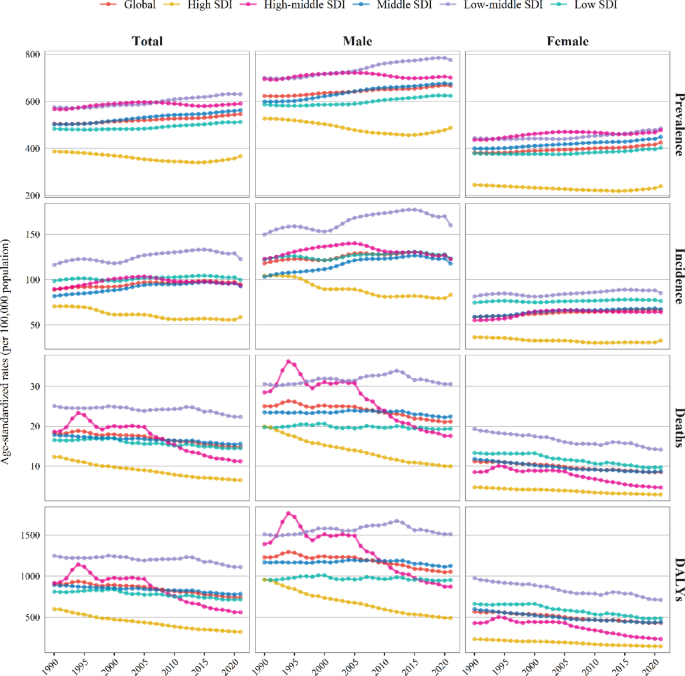
IHD is the leading cause of death among all types of CVD, responsible for the highest number of DALYs, reaching 2,275.9 per 100,000 population, and although it is often considered a condition affecting older adults, the early-onset burden has become increasingly significant. This study provides a comprehensive analysis of the disease burden of individuals aged 15–49 years. The results indicate that though the ASMR and ASDR of IHD among the young and middle-aged population have decreased since 1990, the number of IHD prevalent, incident, death case and DALYs still increasing, and ASPR and ASIR are also on the rise. Notably, this pattern contrasts with recent evidence from older adults (≥ 55 years), where IHD incidence has shown a declining trend underscoring the growing vulnerability of younger populations21. We also found that countries with low-middle SDI had the highest burden in 2021 and the burden of IHD is significantly higher in men than in women. Dietary risks, high LDL cholesterol, high systolic blood pressure, tobacco and air pollution were the most important risk factors for IHD globally. The burden of IHD in the 15–49 age group remains severe and should not be overlooked.
The burden of IHD among the young and middle-aged population shows striking variation across countries at different levels of socioeconomic development, with the highest burden observed in low-middle SDI countries. Health outcomes are closely linked to socioeconomic development, and low-middle SDI regions, which are undergoing modernization and urbanization, often face rapid changes in living environments and lifestyles, leading to increased exposure to health risks, such as sedentary lifestyles, poor dietary patterns, air pollution, obesity, hypertension, and high blood glucose, particularly for the young and middle-aged working population22,23. Consistent with this, the North Africa and Middle East region showed the highest age-standardized incidence and prevalence rates of early-onset IHD in our analysis, likely reflecting the rapid urbanization, dietary westernization, and limited access to preventive care across much of this region24,25. During this process, these countries also face issues arising from relatively underdeveloped healthcare systems, such as inadequate patient education, delayed diagnosis, and insufficient care and intensive care, which prevents them from balancing the growing burden of risk factors26,27. To address these challenges, targeted public health policies are urgently needed — for example, establishing community-based screening programs for hypertension and diabetes, implementing salt and trans-fat reduction policies, and improving access to affordable cardiovascular medications and acute care services. In contrast, high-SDI countries typically have high-quality healthcare systems. In Europe and the United States, cardiovascular disease and major risk factor screening systems have been developed early, allowing for the identification of high-risk populations and early intervention, which reduces the occurrence of acute IHD events28,29,30,31. Similarly, the High-income Asia Pacific region—where the early-onset IHD burden is the lowest globally—has also benefited from comprehensive preventive programs and healthier dietary patterns. In Japan, for instance, nationwide cardiovascular risk screening, along with long-term community-based surveillance, has contributed to sustained control of major risk factors32,33. The well-established emergency and intensive care systems in these regions also significantly reduce mortality from fatal MI34,35. For example, in Italy, despite IHD still being a leading cause of premature death, its mortality rate has steadily declined over the past decade36. Notably, countries with low SDI levels also appear to have a lower burden of early-onset IHD, contributing to the inverse U-shaped relationship observed between SDI and IHD rates. In low-SDI countries, the limited diagnostic capacity of health systems may lead to underdiagnosis, misclassification, or underreporting of IHD, contributing to an underestimation of its true burden37. Civil registration and vital statistics systems are often weak or incomplete, resulting in limited availability of reliable cause-of-death data for cardiovascular diseases38. Moreover, competing health risks such as infectious diseases, malnutrition, and injury-related mortality may mask the actual burden of cardiovascular disease in younger populations39. Strengthening disease surveillance systems, improving diagnostic accuracy, and integrating IHD monitoring into existing public health frameworks would be key steps to improve data quality and inform more effective interventions in these areas.
From 1990 to 2021, advancements in medical technology have significantly controlled the occurrence of fatal events associated with IHD. These improvements have led to better outcomes for high-risk acute events, particularly acute myocardial infarction (AMI). For instance, timely reperfusion therapies, such as primary PCI (PPCI), have become a standard of care for ST-segment elevation MI (STEMI). A study focusing on STEMI patients found that in 37 European Society of Cardiology countries, the number of PPCIs per 1 million population ranged between 400 and 600, with half of the countries showing substantial increases in PPCI utilization over the years40. As a result, age-standardized mortality rates for coronary artery disease have decreased by 30%–60% in high-income and many middle-income countries over the past decade41. These technological advances, particularly in acute care, have significantly reduced mortality from fatal MI. In recent years, the integration of digital innovations, especially the Internet of Things (IoT), has further expanded the scope of cardiovascular care42. IoT-based systems allow continuous patient monitoring, remote detection of arrhythmias, and real-time transmission of critical health data, which enhance early diagnosis, facilitate timely interventions, and may ultimately contribute to improved outcomes for IHD patients. Incorporating such digital health approaches may complement traditional strategies to further reduce the burden of early-onset IHD. In regions with lower SDI, the decline in IHD mortality and DALYs is less pronounced. Patients from these regions often face significant challenges in accessing effective treatment. These include lower healthcare expenditures, lack of insurance coverage, and limited access to life-saving interventions, such as coronary revascularization and heart surgery, which results in higher post-discharge mortality rates43. Strengthening universal health coverage, expanding essential cardiac care capacity, and establishing referral networks for acute coronary events could help narrow these disparities and improve survival in resource-limited settings. While mortality from IHD has been partially controlled globally, the incidence and prevalence continue to rise. In countries with high SDI, where cardiovascular risk factor monitoring and management systems were established earlier, both incidence and prevalence have been largely controlled44. In contrast, countries at other SDI levels are experiencing increases in both incidence and prevalence, which may be attributed to the widespread prevalence of risk factors such as hypertension, diabetes, obesity, and unhealthy lifestyles, underscoring the need to strengthen routine surveillance and early prevention programs targeting these modifiable risk factors45,46.
Gender and age differences play a critical and significant role in shaping the burden of early-onset IHD, with men consistently bearing a far greater burden than women across all regions, and the gap widening with age. In terms of gender differences, men have a much higher burden than women across all regions and age groups, regardless of the level of socio-economic development. Several factors, including genetics, lifestyle, social psychology, clinical manifestations, and healthcare, can help explain this gender difference47,48. Men have a higher proportion of tobacco-related DALYs than women, as they are more likely to be exposed to tobacco. Studies examining the gender-specific associations between risk factors and young people’s AMI have found that current smoking is associated with the highest odds of AMI in men49. Additionally, compared to older women, premenopausal women may benefit from significant protection from sex hormones, such as estrogen and ovarian hormones, which regulate oxidative stress and promote re-endothelialization, inhibiting the development of atherosclerosis50,51. Our results also show that the rising trend in the incidence and prevalence of early-onset IHD has been much faster in women than in men over the past 30 years. This could be attributed to the higher obesity rates in women, as high body mass index is a key contributing risk factor for early-onset IHD, with its proportion increasing significantly over the past 30 years46. Additionally, compared to older women, middle-aged and young women face pregnancy-related risk factors, such as oral contraceptive use, gestational hypertension, preeclampsia, and postpartum depression52,53,54,55. These women are often overlooked, leading to delayed diagnosis, and since women are less likely to experience chest pain and more likely to have symptoms masked by nausea or vomiting, the increasing awareness and improvement in screening systems have led to earlier diagnoses, contributing to the rise in incidence and prevalence, particularly among women56,57. These gender differences become more pronounced with age, peaking in the 45–49 age group, which reflects the cumulative effect of various risk factors over time. We also found that in countries with lower SDI, the control of IHD-related mortality in men is suboptimal. This may be due to lifestyle, working conditions, and cultural factors, with men in these countries facing more risk factors such as smoking, unhealthy diets, and air pollution58. At the same time, these high-risk groups often have limited access to healthcare services, which not only leads to delayed diagnosis but also causes them to miss the optimal treatment window for acute events59. Therefore, when making decisions about the prevention and management of early-onset IHD, it is crucial to consider both age and gender, particularly focusing on gender-specific risk factors and implementing differentiated management strategies. In countries with different levels of socio-economic development, policies should be tailored to local conditions, such as focusing on the female population in lower- and middle-income countries through improved screening for pregnancy-related cardiovascular risks, promoting tobacco cessation and weight management programs, and enhancing access to affordable primary and preventive care services.
Finally, this study identified several modifiable risk factors that significantly affect the burden of IHD among the young and middle-aged population, including tobacco use, unhealthy diet, hypertension, dyslipidemia, hyperglycemia, obesity, and insufficient physical activity. Notably, dyslipidemia and unhealthy diet ranked as the top two risk factors globally and in all SDI regions, which aligns with previous findings in younger populations, though hypertension has a higher population attributable fraction in those aged 55 and older21. This indicates that improving dietary habits and controlling blood lipids can yield significant preventive benefits in the middle-aged and young population and can also improve patient outcomes60,61. Overweight and obesity remain major health crises and are important risk factors for IHD. To date, no country has been able to curb the rising prevalence of overweight and obesity, particularly in adolescents and adults, leading to an ongoing increase in the IHD burden attributable to obesity46. In countries with higher socio-economic development, systems for identifying and treating major cardiovascular risk factors, especially hypertension, diabetes, and dyslipidemia, have been established44. Over the past 30 years, these countries have seen initial successes in controlling these risk factors through targeted primary, secondary, and tertiary prevention policies, though the burden of overweight and obesity continues to rise, requiring more effective prevention and management measures62. In contrast, in countries with lower socio-economic development, which are undergoing rapid transitions, air pollution control is suboptimal. Air pollution is a risk factor for many diseases and may increase the risk of IHD through mechanisms such as oxidative stress, endothelial dysfunction, and vascular dysfunction63,64.
link