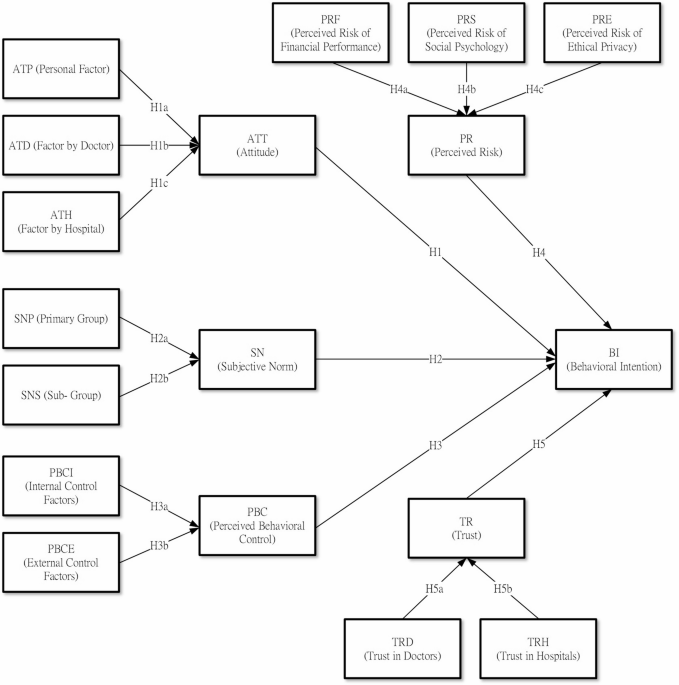
This study offers significant theoretical and empirical contributions by enhancing the understanding of healthcare-seeking behaviors among middle-aged and elderly individuals with critical illnesses. Our expanded Theory of Planned Behavior (TPB) framework incorporates Perceived Risk (PR) and Trust (TR)30, providing richer insights into decision–making processes, particularly during global health crises such as the COVID-19 pandemic. First, our findings highlight that institutional trust significantly surpasses traditional TPB constructs, such as Attitude (AT) and Perceived Behavioral Control (PBC), in predicting healthcare-seeking intentions. This result supports Piette et al. identification of institutional trust as a critical determinant influencing patient decisions during uncertain situations22. Contrary to Gibson et al. balanced view between institutional and interpersonal trust23,24,25,26, our research distinctly demonstrates a more substantial influence of institutional trust, likely driven by concerns over infection control, hospital safety protocols, and institutional preparedness, as echoed by Han et al. during public health emergencies31,32,33,34,35,36. Practically, healthcare institutions should prioritize transparent communication about safety measures, infection control protocols, and emergency response capabilities to bolster patient trust and engagement.
Second, in examining Attitude (AT), hospital-related factors (ATH) emerged as the most influential, followed by physician-related (ATD) and personal factors (ATP). This aligns with Zeng et al. emphasis on the healthcare infrastructure’s impact on shaping patient attitudes16. The heightened importance of hospital infrastructure during the pandemic suggests that healthcare institutions should visibly invest in facility cleanliness, staff professionalism, and quality accreditations to positively influence patient perceptions and build trust.
Third, our findings regarding Subjective Norm (SN) indicate that secondary group norms (SNS), such as peer and community networks, exert a greater influence than primary group norms (SNP), like those of family members. This finding resonates with Bélanger-Gravel and Amireault’s research, reflecting Taiwan’s demographic shift towards aging populations, particularly in “empty-nest” households18. Thus, community-based interventions, including peer education programs, local health forums, and community support groups tailored to older adults, are crucial in shaping subjective norms and promoting healthcare utilization.
Fourth, consistent with McEachan et al. findings, internal control factors (PBCI)—specifically self-efficacy and health literacy—were more influential than external control factors (PBCE)14. Contrary to Shie et al. focus on healthcare accessibility34, Taiwan’s universal healthcare system likely minimizes external barriers. Therefore, interventions emphasizing patient education, chronic disease management training, and health coaching are crucial in enhancing self-efficacy, enabling older adults to navigate healthcare proactively.
Fifth, the influence of Perceived Risk (PR), notably Social-Psychological Risk (PRS), was more pronounced than financial or privacy concerns. This differs from Hsieh et al. emphasis on financial factors3 and aligns with studies by Dryhurst et al., Huang et al., and Han et al., which highlight psychological stresses such as fear and uncertainty during pandemics13,35,36. To address these psychological barriers, targeted interventions are recommended, including:
-
(1)
Transparent communication to clearly articulate infection risks and safety protocols.
-
(2)
Mental health support services are integrated within healthcare facilities.
-
(3)
Crisis-oriented patient education to reduce uncertainty around medical procedures and expected outcomes. These efforts can alleviate emotional barriers and encourage timely care-seeking among anxious or hesitant patients.
Sixth, our comparative analysis across chronic conditions offers additional insights. Patients with hypertension and hyperlipidemia showed stronger associations with healthcare-seeking intentions due to the severity of potential cardiovascular complications. This aligns with findings by Yoshimi et al. and Hsieh et al.3,7. Conversely, patients with hyperglycemia demonstrated weaker associations, possibly due to milder symptomatology, as reported by Chudasama et al.37. Tailored interventions, such as condition-specific education and targeted risk communication, are thus recommended, particularly for patients with less overt symptoms or those with progressive conditions.
Ultimately, our expanded TPB model remains relevant beyond the pandemic, offering a robust framework for understanding healthcare behaviors in an evolving landscape characterized by digital transformation and persistent risk perceptions. Trust, perceived risk, and self-efficacy will continue influencing patient decisions, particularly as telemedicine and AI-based healthcare solutions expand. Hence, integrating ethical transparency, digital health literacy, and system-wide innovations into healthcare strategies is crucial for maintaining patient engagement and trust in the long term22,30.
Limitations and future directions
Several limitations of this study should be acknowledged to enhance clarity and inform future research directions. First, the cross-sectional design restricts the ability to draw definitive causal inferences, and the reliance on self-reported data introduces potential biases, including recall and social desirability biases. Second, although moderation analysis was initially considered to investigate how demographic or contextual factors might influence the observed relationships, it was ultimately excluded due to the complexity and primary focus on mediation pathways.
Future research incorporating moderation analysis could provide valuable insights into factors that strengthen or weaken these relationships. Additionally, longitudinal studies are recommended to better understand how healthcare-seeking behaviors evolve, particularly in response to prolonged health crises. Furthermore, cross-cultural and international comparative studies would be beneficial to identify variations in healthcare behaviors influenced by diverse healthcare systems and cultural norms. Lastly, given the increasing adoption of digital healthcare platforms, future studies should investigate how digital interactions influence trust and perceived behavioral control within frameworks such as the Theory of Planned Behavior. Addressing these limitations will substantially contribute to the development of targeted interventions and policies, thereby facilitating equitable access to healthcare for vulnerable populations.
link