Digital medical management after discharge represents a new approach to chronic disease management, leveraging technologies such as the Internet, mobile terminals, and intelligent cloud platforms10. Compared with the conventional outpatient follow-up mode, this approach has emerged as a cost-effective strategy with expanding utilization across therapeutic applications and is likely to solve many problems such as the low completion rate of secondary prevention of CAD and cardiac rehabilitation treatment11,12. Our research demonstrated that digital healthcare systems can significantly enhance post-discharge management of CAD by reducing the incidence of major adverse cardiac events and ultimately lowering patient mortality through improving lifestyle modifications, controlling risk factors, monitoring medication, etc.
Post-discharge management of CAD typically involves lifestyle improvement, risk factor control, application of secondary preventive drugs and symptom management13. There remain several challenges with the current international application of digital healthcare in the long-term management of CAD. Firstly, only a limited number of mobile health-based interventions have managed multiple risk factors related to CAD, and about 80% only focus on one of the lifestyles, such as diet, exercise, or smoking14,15. The digital management system needs to comprehensively regulate multiple risk factors for patients, including complications, comorbidities, systemic metabolism, psychology, nutrition, exercise, sleep, and other aspects. Only comprehensive intervention can yield greater benefits16. Secondly, since risk factors and conditions vary among patients, personalized management plans, including tailored rehabilitation frequency, intensity, and specific metrics, are essential. However, many digital healthcare solutions still employ a ‘one-size-fits-all’ approach, where all patients follow a similar programme17, and rarely reconstruct personalized content through real-time feedback18. In addition, most digital healthcare trials have focused on patients with acute coronary syndrome or those who have undergone coronary artery procedures12,19, while their application in patients with stable angina, who are often recommended for cardiac rehabilitation, remains understudied. To enhance the overall effectiveness of CAD post-discharge management, future studies should include these patient populations. Finally, most published studies have relied on surrogate endpoints, such as peak exercise capacity and physical activity20, while seldom reporting on more critical outcomes like morbidity, readmission, or mortality17. Consequently, there is a need for more robust data on these reliable endpoints to better demonstrate the effectiveness and value of digital healthcare interventions.
Our investigation has systematically incorporated and optimized the following dimensions to advance post-hospitalization care quality, ultimately demonstrating marked efficacy in mitigating cardiovascular morbidity and mortality rates: 1. Personalization: Recognizing the heterogeneous nature of cardiovascular risk profiles and pathophysiological presentations, we implemented precision medicine principles. Digital health enables highly personalized post-discharge management for CAD patients by integrating real-time data, predictive analytics, and patient engagement tools, with protocol adjustments facilitated through iterative feedback mechanisms. 2. Sustained Longitudinal Care Continuum: Post-discharge management for CAD patients is a prolonged and complex process. However, many studies only cover the first few months post-discharge, failing to provide support throughout the entire follow-up period. This limited coverage often leads to decreased patient adherence and loss of critical medical guidance. Our study implemented a 12-month long-term management plan for CAD patients, continuously tracking disease progression and treatment efficacy. This paradigm ensured uninterrupted clinical oversight, counteracting therapeutic non-compliance and guidance discontinuity prevalent in prior models. 3. Multimodal Patient-Centric Education Framework: Moving beyond conventional SMS-based health communication limitations, which impose excessive reliance on patient autonomy and inadequately convey complex clinical information, we deployed a multi-channel health literacy strategy. Integration of mHealth platforms, dedicated patient portals, social media interfaces, and voice-activated AI systems was complemented by on-demand telecardiology consultations, thereby optimizing therapeutic comprehension and behavioral adherence. 4. Dynamic Monitoring and Feedback: Given the rapid progression of CAD, in addition to active symptom reporting, we utilized daily and professional monitoring devices to track patients’ vital signs in real-time, dynamically monitoring health status. By continuously observing these parameters and promptly alerting medical professionals to abnormalities, potential crises can be anticipated, and adverse events mitigated. Notably, the DM group had more risk factors and comorbidities at enrollment compared to the CM group, as well as worse cardiac function and a higher rate of coronary interventions. Despite these disadvantages, patients in the DM group demonstrated a better prognosis.
Regarding lifestyle improvements, the smoking cessation rate in the DM group of our study was significantly higher than that of the CM group. The smoking rate in the DM group showed a sustained decline throughout the 12-month intervention. In contrast, the CM group exhibited a reduction in smoking rate during the first 3 months, but a slight rebound was observed by the 12th month. At the 12-month follow-up, smoking rates in the DM group decreased by 13.7%, compared to a 2.2% decrease in the CM group. This indicates that the risk factor management in the CM group was less effective in maintaining the reduction in smoking rate over the long term. Moreover, BMI was also better managed in the DM group, with a significantly greater reduction compared to the CM group by the 3rd month, highlighting the early effectiveness of the DM group in weight management. And the BMI in the DM group decreased from 26.45 to 24.95 (mean) over 12 months, while the CM group’s BMI remained almost unchanged. These findings align with the conclusions of previous studies. Smoking is a major modifiable risk factor that should be targeted as part of every primary and secondary CAD prevention programme21. A Meta-analysis on the effectiveness of Internet-based smoking cessation interventions reported that participants receiving the text-messaging programs were almost twice as likely to quit smoking at the 6th month compared with those who did not receive the programme22. Besides, a systematic review evaluating the effectiveness of health apps in managing patients with CAD showed improvements in BMI, waist circumference, and physical activity among app users23.
In terms of risk factors, the systolic and diastolic blood pressure levels in the DM group were significantly lower than those in the CM group at both the 3rd and the 12th month. This underscores the efficacy of digital management in achieving optimal blood pressure control, a critical determinant in mitigating cardiovascular risk. Although the heart rate in the DM group remained elevated compared to the CM group throughout the study period, it demonstrated a consistent downward trend. In contrast, the CM group exhibited a mild rebound in heart rate. This pattern suggests that the DM group’s management strategy may offer greater benefits for long-term CAD management. At baseline, the LDL-c levels in the DM group were significantly higher than those in the CM group. However, the DM group showed a progressive decline in LDL-c levels at both the 3rd and the 12th months. By the 12th month, LDL-c levels in both groups showed no statistically significant difference, indicating that the DM group achieved a more pronounced reduction in LDL-c levels over time. The digital management approach in the DM group also resulted in a significant improvement in glycemic control during the short term. Although the improvement in glycemic control was similar between the DM and the CM groups by the 12th month, the DM group achieved faster attainment of glycemic targets compared to the CM group. This finding suggests that early and rapid optimization of risk factors represents a more effective strategy for CAD management. In addition, the DM group demonstrated significant improvements in both renal function, as assessed by estimated glomerular filtration rate (eGFR), and cardiac function, as measured by LVEF. These findings highlight the comprehensive efficacy of the digital management in addressing multiple risk factors associated with CAD. The observed improvements underscore the potential of digital management to provide holistic cardiovascular risk reduction, enhancing both patient outcomes and long-term prognosis. Consistent with our findings, a recent 3-month digital medical-guided cardiac rehabilitation program reported an average reduction in LDL-c levels of 11 mg/dl24. Meanwhile, the HERB-DH1 pivotal study affirmed the potential of digital management to reduce blood pressure through non-pharmacologic lifestyle changes in untreated patients with primary hypertension25. A previous study on patients with diabetes also demonstrated that digital management tools are effective in improving glycemic control and reducing the risk of cardiovascular events, and have been recommended by the European Society of Cardiology (ESC) guidelines for Diabetes and Cardiovascular Disease26. As for medication adherence, our study also obtained positive results, aligning with the conclusions of several previous studies27,28.
This study is the largest cohort study on long-term management of CAD patients by digital healthcare system, and it is the first article to discuss the clinical benefits of digital post-discharge management on long-term outcomes. Our DM group adopted comprehensive, real-time follow-up approaches that encompassed lifestyle improvements, tighter control of risk factors, increased adherence to secondary preventive medications, and effective symptom management. These interventions ultimately contributed to improved clinical outcomes.
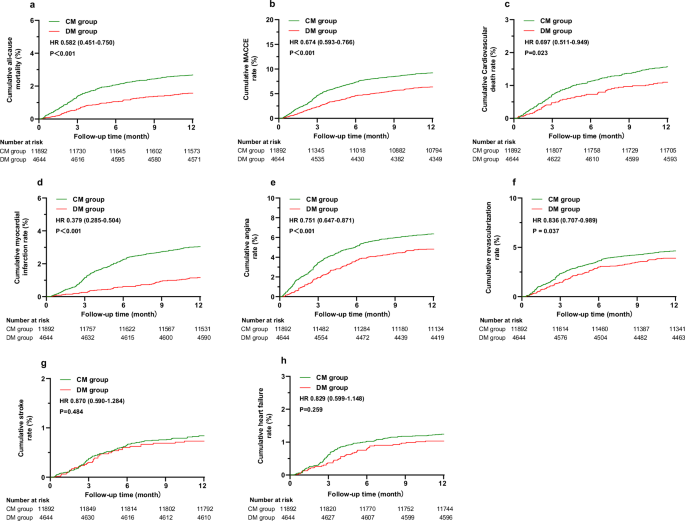
Our analysis demonstrated that the all-cause mortality and cardiovascular mortality in the DM group were significantly lower than those in the CM group, with the effect being more pronounced after adjusting for confounding factors. In the multivariable analysis, the all-cause mortality risk in the DM group was further reduced by approximately 73% compared to the CM group, with a 41% reduction in the risk of MACCE events and a 65% reduction in the risk of cardiovascular disease mortality. Meanwhile, a similar trend was observed in other adverse events, including myocardial infarction, angina, revascularization, and rehospitalization, where digital management effectively reduced the risk of these events. The digital management consistently reduced MACCE risk across all analyzed subgroups, with no statistically significant heterogeneity detected. These findings reinforce its utility as a scalable strategy for secondary prevention. Our findings are consistent with other research findings both domestically and internationally. The TELE-ACS study showed that the approach of telemedicine to manage patients following acute coronary syndrome can reduce hospital readmissions, emergency department visits, unplanned coronary vascularization, and symptom episodes29. A study of patients with chronic heart failure found that remote monitoring can significantly reduce all-cause mortality and hospitalization rate30. The Meta-analysis by Cruz-Cobo suggests that mHealth has a positive impact on CAD patients in activity capacity, medication adherence, readmission, physical and mental quality of life31. These studies support our view that digital healthcare has significant value in the management of chronic diseases. Moreover, there are some potential benefits of our program that are difficult to quantify. For instance, features such as campaign reminders, risk stratification, two-way information exchange, and video education content likely contribute to enhancing the quality of post-discharge management. Nevertheless, some studies have held different attitudes towards digital healthcare management, arguing that it has little significance to the improvement of long-term cardiovascular events and mortality32,33,34. However, factors such as insufficient sample size, short follow-up duration, and inadequate management may have hindered the overall improvement in these studies.
Digital health management has demonstrated efficacy in managing various chronic conditions35,36 such as diabetes, obesity, and chronic obstructive pulmonary disease (COPD), with its application in CAD offering unique advantages. In CAD management, digital health platforms facilitate continuous remote monitoring of vital signs and symptoms, enabling early detection of exacerbations and timely intervention. This real-time data collection enhances risk stratification and personalized treatment plans, improving patient outcomes. Moreover, digital tools promote medication adherence through reminders and educational content, crucial for secondary prevention in CAD. They also support lifestyle modifications by tracking physical activity, diet, and weight, integral components of cardiac rehabilitation. The integration of telemedicine allows for regular virtual consultations, reducing the need for hospital visits and enabling healthcare providers to adjust therapies promptly. Data analytics and artificial intelligence further refine CAD management by predicting potential adverse events and optimizing resource allocation. Patient engagement is bolstered through interactive platforms that encourage self-management and provide psychosocial support, addressing the holistic needs of individuals with CAD. Interventional cardiologists can leverage digital health technologies to enhance patient management by optimizing post-procedural care and delaying the progression of arterial restenosis, thereby reducing the necessity for repeat interventional procedures. Through continuous remote monitoring and timely early intervention, they effectively minimize hospital readmissions caused by disease exacerbation. This proactive approach enhances the utilization of healthcare resources, ensuring that they are allocated efficiently and effectively to improve patient outcomes and streamline the healthcare delivery process. In essence, digital health management in CAD offers a comprehensive, patient-centered approach that enhances disease monitoring, treatment adherence, lifestyle intervention, and predictive analytics, ultimately leading to improved quality of life and reduced healthcare costs. Given its convenience and scalability, further promotion and integration of digital medical technologies in clinical practice have great potential to optimize long-term CAD management.
This study has several limitations. First, this research is an observational study, which inherently carries limitations. Observational studies are prone to confounding factors and cannot establish causality. The lack of randomization may result in unmeasured variables influencing the outcomes, thereby limiting the generalizability and robustness of the findings. Secondly, from the perspective of baseline characteristics, there is a potential for selection bias. Participants in the DM group were older, had more comorbidities, and exhibited poorer baseline cardiac function. These factors may have driven a greater urgency for post-discharge management guidance and a stronger willingness to participate. In contrast, the CM group consisted of younger patients who may have had insufficient awareness of disease management, limited time and energy, or concerns regarding privacy. These disparities in baseline characteristics could skew the results, as the DM group might inherently benefited more from structured interventions. Therefore, in light of the above, future studies should consider designing and conducting randomized controlled trials (RCTs) to minimize bias and unify baseline differences, which could provide a more comprehensive understanding of the true impact of digital health management in CAD patients. Thirdly, the digital management system used in this study requires further enhancement, such as integrating more wearable devices for comprehensive monitoring. With the rapid advancement of AI, a more sophisticated management system is expected to achieve better outcomes. Finally, this study is primarily based on patient data from China, and the results may not be fully generalizable to patients in other countries and regions. Therefore, future research should be conducted across different populations and regions37 to validate the effectiveness of digital healthcare.
In conclusion, this study indicates that digital healthcare offers significant advantages over conventional follow-up mode in the post-discharge management of CAD patients, effectively optimizing lifestyle, reducing risk factors, and improving patient prognosis. Our study highlights the significant reduction in all-cause mortality in patients with CAD. These findings underscore the potential value of digital healthcare in enhancing outcomes for CAD patients. Future research should continue to explore the impact of digital healthcare across diverse patient groups and regions to further validate its role and value in the management of chronic diseases.
link